Introduction to Air Decontamination, Infection Control, Future Business Bio-Resilience
Whether one is protecting from bio-terrorism, or more common Airborne Respiratory Illnesses (ARIs) such as Tuberculosis, RSV, Influenza, or COVID-19, or Fungal Spores, the breathing of clean, uncontaminated air is fundamental to preventing or controlling the risk of catching these debilitating and deadly diseases in the first place.
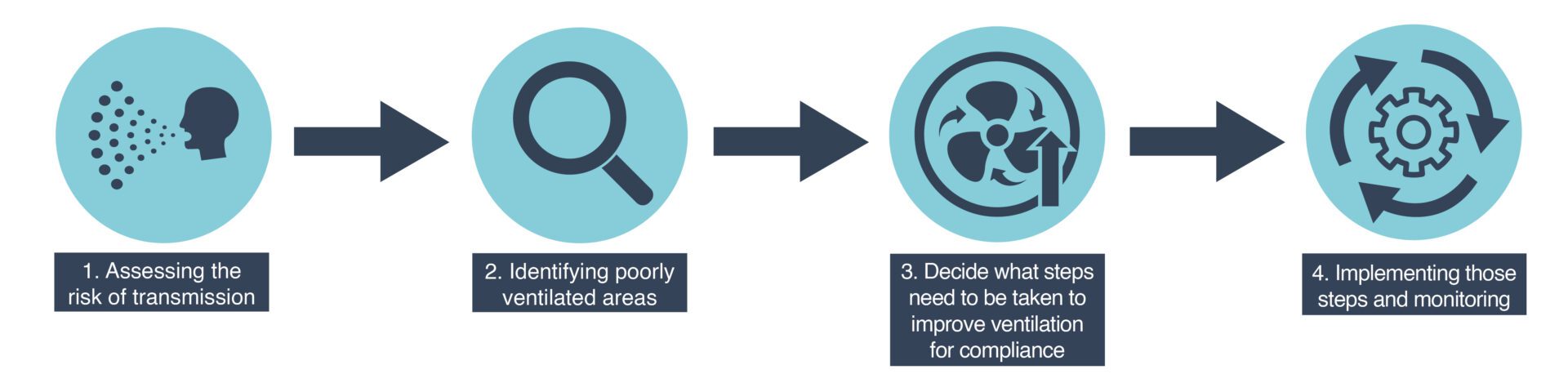
For common respiratory diseases, one should think broadly of the “80:20 Rule” to prevent and control infection – spend 80% of your efforts on improving ventilation and air purification and 20% on cleaning surfaces (See below).
ARI risk arises when an infected person exhales, talks, coughs, sneezes, and sings because the hazard is carried in their contaminated breath for hours after being exhaled into the air. Infection risk is more significant among people indoors. The good news is that ventilation and air filtration strategies can significantly help reduce biological particle concentration, also known as bio-load. The lower this concentration, the less likely such infectious particles can be inhaled into the lungs of other occupants; less exposure to eyes, nose, and mouth; and importantly too, less bio-material falls out of the air to accumulate on surfaces. Protective ventilation practices and interventions with air filtration will significantly reduce the airborne infectious aerosols and reduce the overall infection risk to occupants.
Dring Covid we were told, “we have to learn to live with the virus”. We do not accept this statement. We can do much better than this! With the correct Engineering & Technology interventions, we can protect and Build Back Better than pre-Covid, ready for whatever might come next.
Indeed, if we have clean air to breathe, we are confident, healthier, more mindful, and our cognitive capacity is much higher. With improved interior air quality and infection suppression controls, it is not just about Covid-Delta variant prevention and control; we are protecting better from the risk of other variants, other pathogenic spores, bacteria and viruses. We create sustainable long-term protection from all common pathogens within the built environment and transport systems.
PP-L are able to create not just infection resilience for their clients but also, long-term, Pandemic Resilience with sound advice and providing the appropriate safe Engineering & Technology solutions to achieve this level of protection for any given interior environment.
Compliance
Let us not ignore compliance either. Ventilation in the workplace should be assessed and improved alongside other measures to reduce the risk of a biological agent or pathogen exposure. The Workplace (Health, Safety and Welfare) Regulations 1992 and the Workplace (Health, Safety & Welfare) Regulations (Northern Ireland) 1993 require Employers to ensure that there is an adequate supply of fresh air in enclosed workplaces. The term fresh air means that it must be clean, uncontaminated, and unable to cause harm.
In the pandemic era, the law and associated regulations give most of the conventional mechanical ventilation systems within the Built Environment a difficult compliance challenge because most of these air filtration and ventilation systems recirculate part or most of the air extracted from a room back into that and other interior spaces. With adequate ventilation, one decontaminates a space by removing that exhaled air quickly to the outside. Whereas for any form of the recirculated air system, one is recirculating and re-distributing potentially bio-contaminated or infected air.
To ensure compliance with the Workplace Regulations, etc. – Employers and those in control of premises need to assess ventilation in the workplace. The regulations and guidance confirm the need for “adequate ventilation” but are not specific about what that exactly means. Many regulators and advisory institutions around the world indicate that adequate ventilation is:- the greater of 10 litres/person/second or 6 Air Changes per Hour (6ACH) of clean, uncontaminated air as the minimum, but these rates need to be greater if the environmental conditions, occupancy or risks dictate otherwise.
These are all the areas where PP-L Biosafety can help you to protect your people, visitors and business operations to levels exceeding compliance, to better normal and for the long-term.
Our Services and Products give our clients an advantage in their marketplace by preventing or controlling the risk from all common pathogens, including coronavirus and protecting your people and business operations better to withstand whatever may come in the future.
Why is ventilation important?
Good ventilation reduces the concentration of viruses in the air and therefore reduces the risks from airborne transmission. Airborne viruses can be contracted through inhaling small particles (aerosols) in the air after someone with the virus has occupied an enclosed area.
Unfortunately, few indoor environments have been designed with consideration for the risk of a highly infectious viral pathogen and so reliable and safe ventilation systems which are suitable for infection prevention is not always achievable using existing systems.
Cold weather also aids the transmission of airborne viruses such as COVID-19 and so attempts to ensure ventilation may not necessarily have the desired effect.
There are also important weaknesses which must be considered and opportunities for improvement in many systems.
What is “Adequate Ventilation”?
To reduce the transmission of COVID-19, Influenza and common airborne pathogens within indoor environments, the term “adequate ventilation” is used by some regulators. Others are clearer in their guidance, and we recommend the following, having reviewed positioning, globally:
1
Ventilation systems must draw as much clean outdoor air into interior environments as possible to dilute and replace contaminated and exhaled air. Take measures to filter air pollutants out adequately, especially in built-up areas or those with an API of 50 or more.
2
HVAC systems should utilise the best quality filters that are practicable, given the constraints on plant capability, capacity and maintaining airflow velocity. If humidity can be adjusted, target 40-60% relative humidity to reduce risk of infection.
Recirculation ventilation systems should be set to full fresh air flow to avoid re-distributing infected or contaminated air back into rooms; otherwise, deploy in duct Germicidal Ultraviolet (GUV) to supplement more conventional building filters; or upgrade to MERV13 to HEPA Filters range to protect from coronavirus.
3
For whole building protection, Engineered GUV devices should be deployed in the HVAC duct, near the filter and coils, to suit the duct size, airflow velocity (contact time), temperature range, humidity, target microbe and target inactivation level (i.e. clean, disinfected or sterilised air).
4
Mechanical Ventilation Systems should maximize the number of air changes in each room per hour to remove harmful contaminants including infectious particles. We recommend a risk-assessed approach to suit use, ideally achieving the greater of 6 Air Changes per Hour (ACH) but not less than 10 litres/person/second occupancy level.
Higher Risk environments will warrant higher ventilation air flow rates and different filters. For new buildings, MERV13 filters can be specified, but the plant and energy needed will be more expensive in terms of capital and operational costs than conventional filters and GUV. Upgrading filters to MERV13 or higher within most conventional existing buildings’ mechanical ventilation systems would probably require a major system refit or upgrade. Air distribution is just as important as the design flow rate.
5
If 6ACH cannot be achieved, or viral load risk is potentially high, or if air flow or air distribution is inadequate, then mitigation should be installed. The space should be protected with correctly specified and positioned fan-assisted GUV upper room/ceiling emitters; or medical grade HEPA Filters with integral GUV air disinfection.
6
In complicated or very high-risk environments, using CFD (computational fluid dynamics) modelling to predict airflow, distribution, dead zones and aerosol generation mapping can be of enormous benefit to engineer targeted ventilation solutions and UV-C interventions.
7
Deploy carbon dioxide (CO₂) monitors or testing. Locate away from doors and windows, ideally at breathing level and at least 0.5 metre away from people as a surrogate measure to identify inadequate ventilation. History demonstrates that improving the building ventilation to a rate which regularly achieves a CO₂ concentration of 600 PPM significantly reduces the transmission of airborne diseases. A figure of 800PPM would be an indicator of “adequate ventilation” or reduced risk. Above this level – call us for free advice.
Mechanical Ventilation
– Recirculated Air HVAC Systems
Heating, Ventilation & Air Conditioning (HVAC) systems which re-circulate air in buildings, in full or in part, are the most common form of ducted systems in the world.
However, studies have shown that these carry a risk of increasing viral transmission rather than decreasing it. This is particularly the case in confined spaces because the potentially infected human exhaled aerosol from occupants is inevitably collected by the ventilation extraction system. The air currents then carry this aerosol through the ducts, where it then passes over heater/cooling coils before being re-spread in the room and indeed, other rooms, spreading microbes even more rapidly.
The viral load generated by occupants of an environment builds over time, unless it can be diluted by introducing more outside air, and HVAC systems can give a false impression of air purity while also accelerating the spread of a virus.
– All Mechanical Ventilation Systems
A considerable draw-back of all mechanical ventilation (recirculated or fresh air) systems is that a biofilm can gradually build on the coils and filters over time, significantly reducing their energy efficiency. Caused by microbial growth, biofilm can be prevented by irradiating the coils using GUV lamps which can also inactivate airborne microbial hazards within the system, disinfecting airborne contaminants that are not caught by the pre-filter through exposure and eliminating surface growth.
A recent study by McKinsey & Co confirms that upgrading HVAC systems by incorporating higher-grade filters can be very expensive and unfeasible in some situations. What’s more, even the very best medical grade HEPA filter will not eliminate the hazard concerns of viral airborne transmission.
Due to the shortcomings of HVAC systems, GUV is often used on spacecraft and submarines along with high quality filtration.
Existing HVAC systems can be upgraded to improve viral-security using UV-C but this cannot be achieved through upgrading filtration alone.
Air Purification – HEPA and other filters
Air filters are used in modern ventilation systems or in portable air purifiers. Filters help to intercept small particles such as pollutants, pollen, dust and some microorganisms, but even high-quality filters will not intercept all viruses sufficiently.
However, if filters are supplemented with competently engineered GUV filaments within the ductwork, these systems can be very effective interventions to mitigate infection risk from all airborne viral hazards.
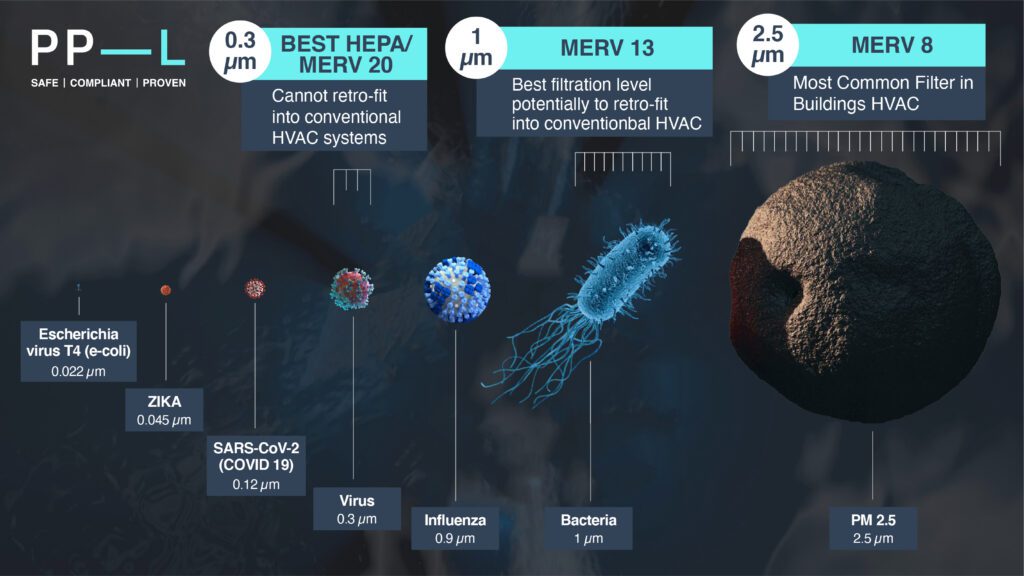
Here are some examples of filters and pore sizes of the filter holes:
Portable Medical Grade Air Purifiers
The majority of so called, “air purifier” devices are basic air processors which only remove larger particulate matter from the air but not all small bacteria and viruses. hpwever this being said they are good for overall IAQ
Our purifiers are the highest efficacy level of medical grade quality. These portable air purifier devices have been proven to be extremely effective at stopping infection in hospitals in Northern Europe and now, we have a sole distribution agreement to supply these potent infection intervention products in the UK.
Our portable air purification products are ideal for inside clinical and high-care spaces such as hospitals, GP surgeries, dental clinics and consulting rooms, as well as conventional spaces such as offices, meeting rooms, cafes, pubs, restaurants, changing areas, lobbies, etc. The PP-L devices will also purify air at an industrial rate such is the quality of the Scandinavian Engineering and a single device is capable of rapidly purifying the air in spaces up to 300 m2.
All CE Marked, ISO 9001 and ISO 14001, as all our products.
In terms of maintenance costs, these devices can safely operate for up to 20,000 hours (c.2 years) constantly-24/7 between HEPA & UV lamp changes which give these devices the lowest level of whole-life costs.
For larger rooms and whole buildings, we can go to an industrial scale of air purification with our fixed fan-assisted upper room GUV devices and HVAC engineered COVID-19-Secure air disinfection solutions.
What is Germicidal UV (GUV)?
Germicidal UV-C or GUV for short is a particular type of invisible short-wavelength ultraviolet light (254nm) which is naturally produced by the sun, although it does not normally enter the Earth’s atmosphere. For more than a century, GUV generated through properly engineered emitters has been proven to kill or inactivate microorganisms including viruses by destroying nucleic acids and disrupting their DNA and RNA.
The effectiveness of GUV has been demonstrated against highly infectious airborne diseases including tuberculosis, measles, SARS and COVID-19, which can be destroyed within milliseconds through exposure to GUV.
How does GUV destroy Pathogens?
PP-L’s GUV products have been developed over 80 years at our Swiss manufacturing facility. With over 130 global patents built up since 1939, the products rely on the trusted blend of gasses in quartz glass tubes to produce the most effective antiviral GUV light on the market.
GUV light is a non-ionising form of radiation with a wavelength between 200nm-280nm, our products produce a wavelength of 254nm – the optimum wavelength for destroying microorganisms – and our products are also non-ozone producing, unlike some UV products.
GUV light is also known as germicidal ultraviolet irradiative light (UVGI) as it destroys the DNA and RNA of microbes by breaking bonds between the thymine and adenine pair and bonding two adjacent thymine nucleotides together. This instantaneous inactivation process stops the exposed microbes from undergoing mitosis and causing harm whether they be in the air, on surfaces or in liquids.
The inactivation solution depends on the medium, environment, hazard source, presence of people or animals, temperature, humidity, bio-load (viral load), exposure time and target microbe that one seeks to eradicate.
Our GUV antiviral air treatment solutions were rapidly and successfully deployed during the first SARS crisis in 2003 for hospitals, environments which are amongst the highest infection risk settings.
Is GUV tried, tested, proven and endorsed?
GUV has been used for more than a hundred years to treat and prevent contagious diseases and there is a wealth of evidence going back decades to demonstrate GUV efficacy in the inactivation and destruction of all known microorganisms. These include highly contagious airborne viruses including COVID-19.
Our GUV products have been proven to inactivate over 35,000 different microbes. The irradiation energy required to inactivate these microbes and other relevant biohazard information are stored in our database, which is one of the largest private databases of its kind in the world. We have our own laboratories and partner with other scientific institutions.
We also possess approximately 4,500 peer reviewed scientific papers which support these conclusions and several studies since the start of the COVID-19 pandemic have demonstrated that GUV is highly effective in quickly inactivating SARS-CoV-2 (COVID-19) to prevent its transmission.
Airborne Transmission of Covid-19
Studies have shown that COVID-19 is capable of remaining airborne for up to 16 hours, travelling tens of metres through the air in an indoor environment, particularly when the air is cold. Studies have also shown that inhalation is the most common means of transmission, with 57% of people being infected in this way, compared to 8% who are infected through contact with surfaces.
Professor Donald Milton, an aerobiology expert from the University of Maryland, was instrumental in the World Health Organisation (WHO) announcement in July 2020 that COVID-19 can be transmitted via the air. He underlines the importance of swift action to prevent airborne transmission in indoor environments: “We need to subsidise bars and restaurants to stay closed. We need to increase ventilation where we can and start making as widespread as possible use of air sanitation with upper-room germicidal UV and maybe far UV in those places that must be open, like elementary schools. We need to stagger hours of starting work and keep density on public transport low, or open windows. And we need to wear masks”.
The science behind GUV is well documented and widely acknowledged around the world. Please contact us for links to some of the hundreds of scientific papers that we have and continue to assemble on the efficacy of GUV as a highly effective infection intervention against COVID-19. These include papers on the human aerosol transmission routes, and papers on various forms of ventilation and their strengths and weaknesses.
For more information on how PP-L Biosafety can help your organisation to improve air security to prevent the transmission of germs and viruses, please contact our team.
Germicidal UV Air Cleaning Devices
Our proven GUV biotech air treatment solutions were utilised to great success during the first SARS crisis in 2003. The current Coronavirus, SARS-CoV-2 is much easier to destroy with GUV irradiation than its SARS-CoV-1 predecessor, whether in the air or on surfaces.
PP-L is able to provide bespoke engineered solutions with GUV for whole buildings and at an industrial scale for spaces both with and without HVAC ducted systems, re-circulated air systems, or in spaces with poor ventilation. We also offer portable Air Purifier Products that combine the use of HEPA filters and GUV that are specified for smaller spaces.
Our GUV technology and GUV-HEPA Purification products are very economical to buy and maintain because the lights themselves are relatively inexpensive and they are highly efficient at inactivating microbes for around 12,000 hours at best efficacy. When our light fittings are changed, there is a very low risk to the person changing them or filters behind them, as all microbes within its vicinity would have been inactivated by the light prior to it being changed.
| Air Purifiers | Our GUV & Air Technology Products | |
| Able to remove microbes of any size | X | ✓ |
| Low risk to change filter | X | ✓ |
| Does the system remain effective for over a year | X | ✓ |
| Are they non-chemical and cheap to run | ✓ | ✓ |
| Can they disinfect against all viruses in the air | X | ✓ |